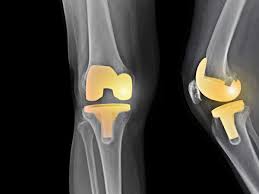
For the last 10 days I have been immersed in the medical world. Roberto had a total replacement of his right knee, and given the state of hospitals these days, they sent him home that same afternoon. From that moment he was mine. We went home with bags of supplies – six different pills, two of them opioids, two kinds of dressings, ace bandages, compression stockings, syringes, alcohol swabs, waterproof pads, two styles of ice packs, elastic straps with the strongest Velcro I have ever met, plastic containers of various sizes and shapes, including the one for disposal of used hypodermic needles – and sheaves of instructions for patient care and an equal number of warnings about what could go wrong.
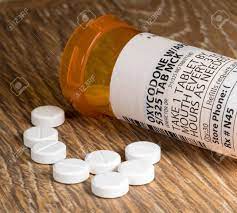
It was frightening to find myself in a profession that I had not chosen. Nursing, in fact, had never even been on my list. I told Roberto that I would do the best I could, and he pledged the same, to do the best he good as recovering patient. But what if something bad happened on my watch? For instance, what if he falls? On Day 2, with me watching, he fell off his crutches, landing backwards, thank God onto the carpet. Or, what if he overdoses on opioids? On Day 4 I lined up the oxycodone pills by the bed, one to be taken at 10:00 pm, the next one at 2 am. Understandably fuzzy-headed from the drugs, he took them both at 10:00 p.m. In a panic I called the National Poison Control Center to report an overdose, and was on hold an agonizingly long time while they did some research, finally assuring me that this was “probably” not dangerous. What if I forget to give him medications on time? That has happened more than once. Sometimes, I confess, sometimes I don’t.
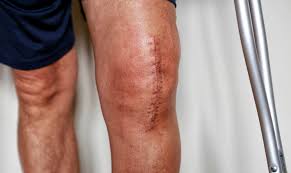
I’m happy to report that despite the mishaps he is doing really well. His physical therapist who comes to the house three times a week says he is right on track and making good progress. The occupational therapist was happy to spot a throw rug that she could condemn and remove, but saw no need to return after Roberto demonstrated skills on the walker and the crutches. At the two week mark we will return to see the surgeon, have x-rays taken and, and for me to receive my care giver commendation… not really, but it will be a milestone. I will feel more or less off duty after that.
There have been important revelations along the way. Top of the list is how lucky we are. We live in a place where this kind of surgery is possible, giving Roberto a future with a pain-free knee. The medical professionals and therapists have been not only highly skilled but encouraging and compassionate. I have made phone calls with stupid questions, the same question more than once, and always been reassured with kindness and patience. I am grateful they chose the career they did, because they are really good at it. And we are so lucky to live in this little community nestled outside Santa Fe, with neighbors who are generous and creative in the ways they support us.
I’ve also learned that caring for a loved one is complex. I’m not the outside skilled caregiver who comes in with expertise and authority to assess and give instructions. I’m the partner bringing a ton of baggage – some wonderful baggage, some not so wonderful – to the situation. I can dish out lots of love, but I can also lapse into fussing and micromanaging, which is not helpful.
It is also impossible for me not to identify keenly with Roberto and what he is going through. The morning after the surgery I woke up with an aching right knee. There were other symptoms that I mimicked that I would rather not talk about. And when I am talking to a nurse or therapist on the phone about how Roberto was doing, I find myself saying, “We’re taking 5 milligrams every 4 hours,” or “Now that we’ve finished taking the anti-biotic, we’re not nauseous anymore.” It’s ridiculous, but I can’t help myself. We’re in this together, doing the best we can.

Wow. Sending heartfelt wishes for a speedy recovery to you both. And a shoutout to all caregivers. It’s challenging on many levels. Great post.
Thank you, Anne. And you know whereof you speak!
Lucy, you manage to see the humor and humanity in any situation.
(Gratuitous advice: Try making an Excel spreadsheet to track how often?/what time?/with foods?/how long?…)
…excel spreadsheet… not a chance! I know they are great, but my spiral notebook is all the technical challenge I can take right now! thanks anyway, Tyson.
Good luck to you both! I can’t get mine done because I’m too old to leave right after the operation, so this info was very interesting. Patience is not my forte and I don’t see JIm as a nurse… so I’ll keep putting it off…tra la…
I know you need and deserve a new knee and am so sorry that you can’t get one asap. As for Nurse Jim, maybe I should start a consulting business for non-nurse care-givers… or on second thought, having re-read my blog, maybe not. Hang in there, and hopefully hospitals will open up and you can on the schedule. A few days ago I would have said, forget it, but today, Day 13 things are really looking up.
What a great blog Lucy! How lucky you are to have each other!
And how lucky we are to have you, dear Dotty, as our trail blazer! Your walker, crutches, shower seat, and great tips have been invaluable.
Oh, dear Lucy! And yet I found myself chuckling as I read your care giving account. You have such a great outlook and sense of humor. We do hope Roberto continues to heal well and quickly. Love to you both, Pam
Thank you, Pam. Glad to give you a chuckle! Love to you and Ken.
You’re both fortunate in your compatibility. I bet with your newly acquired nursing skills you may be considering a new career path?
Very funny, Jamie! Although I am considering a consulting business on the side for the “care-giving challenged” like myself who could use support and a few laughs.
Being a nurse myself (40 years) and have 2 knees and a hip replacement, I know what he and you went through. I also know that the surgeon would not have sent him home right after surgery if he did not think Roberto would be ok and recover fine. I know what a stressful time it was since you were (sort of) unprepared. Were there any pre-surgery class on what to expect pre, during and after surgery and home recovery?
Yes, we had a two-hour orientation session before surgery — everything I needed to know (and forget)! Seriously, it was a big help. The surgery process here is a well oiled machine, and we are so grateful.
Oh Lucy! My mom sent me this today and I had such a belly laugh. Not to laugh at your or Roberto’s expense, but just how relatable this story is to my own with my mom and husband this past June. If you’re ever in need again (which I hope you aren’t) you should check out the medication app “My Med Schedule Plus” for your phone. It has gotten me through two surgeries in 8 months!
You’re an exceptional caregiver and Roberto is lucky to have you! If you’re ever in need, I think my mom is the BEST. We’ll ship her your way 😉 Biggest hugs to you both!!! Leslie
Thank you, Leslie. Yes, tell you mom to have her bags packed. She would be a great nurse…. and she I could do some serious catching up and moderate partying! Love to you all. Take care!
Hi Lucy – i’m a former nurse-midwife/epidemiologist. and furthermore, have had my left knee and right shoulder replaced. they do get a person up and moving as soon as possible – and much to the plus side as this movement gets the healing going and the circulation too … anyway. Bless you for your care giving … I had good friends stay with me for a couple of days after i had those surgeries .. and boom. it worked! and hooray for the PT folks who come out on house calls. THE BEST!!! wishing you and Roberto the best
You are an expert many times over. So glad your experiences were so successful. Roberto is graduating to the cane today — big step!
Hi Lucy,
You are doing great. You are in a very difficult position nursing your life partner. Don’t get stuck worrying about the small stuff. Love and watchful care from the heart is the best thing you can give.
I have been critical care and emergency nursing for almost 40 years and that did not prepare me for helping my mom with my dad. He went through the stages of Alzheimer’s in front of us for 4 years while we cared for him. He finally died from the disease at home a year ago. I was helpless at times too and I am we trained.
You both are succeeding. You get to do it at home away from Covid. And you are lucky that he had both knees done at the same time so you don’t have to go through this twice.
Well done Lucy.
Thank you, Karen, for your wise and compassionate words. “love and watchful care from the heart” — beautifully said. And sorry if I misled you… we will be doing the left knee in a few months!
Part two!
Yep! This has all been a rehearsal.
Sending love and healing wishes for a speedy and successful recovery! Take good care of each other! Xoxo
Thank you, Lucy. Sending much love to you and yours.
Cheap weekly pill sorters work wonders for keeping track. Not even remotely technological! Available at the Dollar Store! (Albeit with guilt at buying cheap plastic from overseas.) I have one with three compartments per day. AM and PM vitamins, for me – opioids for your “we”! You could re-label as needed.
Aha! now that sounds within my skill set. Thanks, Sharon.
My second knee replacement was supposed to be a day trip – my orthopedic doctor does almost all of his on a day basis even before the pandemic made hospitals shorten the stays – mine was Dec 2019. I did stay overnight because mine was more complicated than the usual because they had to take out a mending place from a previous break – only one overnight – and the nurses and PT are much less accomodating that you probably are – they made me get up and walk around the nurses area within 2 hours of waking up in my room and several other times that afternoon and the next day til release. And you probably were more amenable to coming when called – even before the pandemic unless you pushed some emergency button it could take a long time to get a response and even then they were so much more by the rule on pain killers.
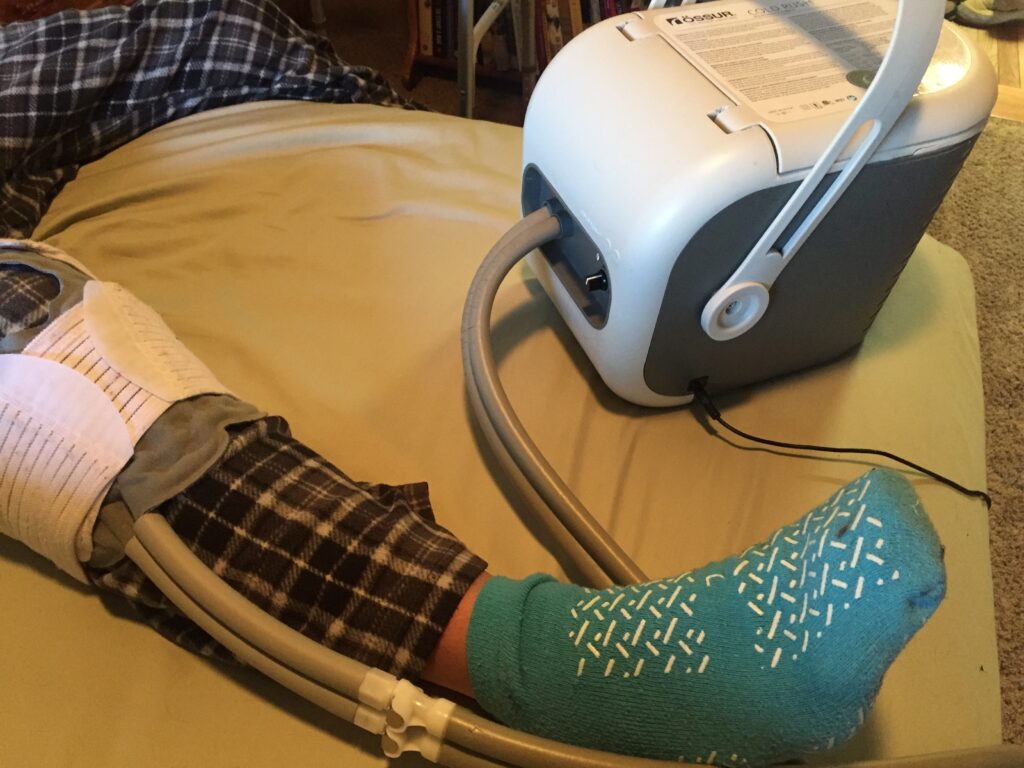
I did end up making a hand drawn table for the meds – my husband isn’t Excel trained nor really trained to track meds. And I loved, loved, loved the cold machine – it was useful for weeks and weeks – in fact I still have it just in case (the price to buy or rent was about the same). I empathize with the caregiver thing – its rough with the anxiety to get it right, but know that even trained nurses cannot always do the A+ job either. Take care of yourself. Roberto will be much more able to take care of himself in a few weeks, although you will be designated driver for more time than you are used to.
Yes, Roberto was up and walking, climbing stairs with crutches, doing all kinds of tricks, two hours after waking up from surgery. They had pumped anesthetics in the site before closing him up so he felt great. And then, the next day when all that had worn off, it was a different story. But clearly the worst is over. Today, two week anniversary, we went to buy a cane — and I mean”we” as in both of us got in the car and went shopping. That was a great step forward. Glad your replacement adventures are behind you!
Lucy,
What an amazing piece you have written about a challenging situation! I love how you are vulnerable and humorous in your writing. Caregiving is not for the faint of heart. I’m sure you are handling it much better than you know.
Sending much love to you. Wishes for a complete recovery to Roberto!
Julie
thanks, Julie, warm words much appreciated.
Thank you for sharing this Lucy, and thank you for doing so in such a timely manner! My turn comes next month when David has a total ankle replacement. I wish you and Roberto much progress in the next months and blue skies thereafter!
You know how to reach me! Best of luck. I’m sure you will both do great.
I am having a belly laugh along with Leslie!!!! I can so relate! Four years ago my husband and I moved to Silver City NM from Phoenix to help my aging parents here. Little did we know that my step dad would be diagnosed with pancreatic cancer and that COVID would descend, which, for the time being, wiped out home care here. My mom and I, with our pen and spiral notebooks, listed medications, chemo appointments and medical equipment as we are not spreadsheet savvy.
And the machine not working in the off position (how dare it!) is priceless! Yup, same thing happened here!
My step dad passed away and now my mom has moved back to Phoenix for health reasons all in this past year. The bond of hands on care that my mom and I share is something I wouldn’t trade for anything.
Your gift of vividly sharing experience is also something I am grateful for, Lucy. It has helped me smile and believe that life has beauty in all kinds of circumstances.
Thank you, Karen, for the highly relatable story.
Lucy, I hope Roberto’s recovery goes smoothly. This 10 days is rough, for you too. In 10 months it will be so worth it. My best backpacking buddy has had both knees replaced and he is so happy about it now.
Thanks, Brian, for the encouragement. Yes, “we” seem to have turned the corner, now on day 15 so I think you are exactly right.
Hey sweet friend – boy do I hear you; David had a spinal fusion in late October – 36 staples, 6 plates, several pins and a long recovery; he’s now in physical therapy but it’s been a slow go. Caregiving is HARD! I’ve lost my patience on more than one occasion 😉 love and hugs from Texas, Susan
OMG, what people go through that we don’t even know! That sounds like a very rough road for you both. So glad he’s in PT and the load is lighter for you… I hope!
Dear Lucy and Roberto – my new year’s resolution was to read less email – and so I missed your blog!! This is a lesson about at least skimming email more often. Although I knew about the knee replacement I had forgotten the when of it. I am so glad to catch you now, several weeks out, and know that all is well. I know a little about at home care giving and how stressful that can be, managing meds and worried about progress. I also know you, and have not a doubt that you did a fabulous job. With 2 new knees Roberto will be hiking and pain free by summer. What a difference it makes to be pain free!! Much love – Kay
Thank you, Kay… and you’re not at all late to the party! It’s only been 16 days, but who’s counting? The good news is he’s now using a cane and we’re even planning a shopping trip today. So the future looks bright! Soon we’ll be in Albuquerque to meet you for lunch at Duran’s. Hope all is well with you and I applaud your less email resolution. Love to you and Dick.
Hi Lucy,
I absolutely love the way you write. Having “been there”, I can only applaud both you and Roberto. To use a great colloquialism, “you done GOOD”. It sounds like Roberto is well on his way to a happy hip. For sure he knows you are really ah angel.
Hugs!
Carolyn (“Lyn”)
Great to hear from you, and so glad it all rings true. It’s his knee and it is happier by the day… and then there is the other one. Maybe in May.